In Thy Mother’s Arms: How Nzara Became a Beacon of Hope for Newborn Health
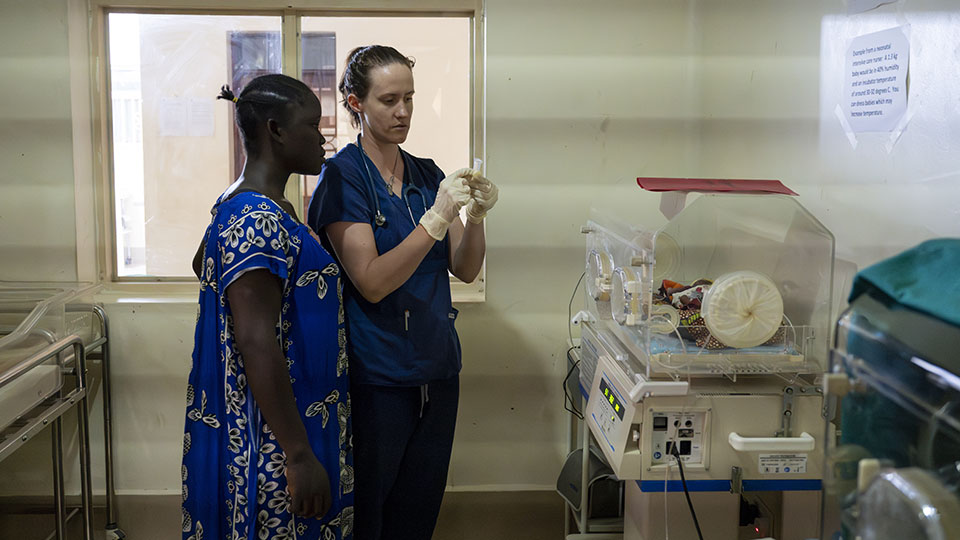
Sometimes, a mother never hears her baby’s heartbeat. Sometimes, a mother never feels her baby move. Sometimes, a mother never witnesses her baby’s first breath or first cry. Sometimes, a mother never gets to leave the hospital with her baby wriggling lively in her arms, but instead must walk home, wailing, pressing her infant’s lifeless body close to her heart. As a nurse-midwife volunteering several times in Nzara, South Sudan over the past five years, I have seen that these ‘nevers’ are common in a world where life and loss walk hand in hand.
I was there during the last moments of 52 little souls during the previous nine months of my most recent volunteer service. This number is far greater than my mind can ever truly process. I remember a specific moment before we had reliable power at the hospital. I was wrapping a baby boy up in a blanket shortly after he had passed away from complications due to lack of oxygen before birth. It felt like a punch to the gut: I was getting too good at wrapping babies in shrouds. And if I was getting too good at it, I couldn’t even imagine the level of loss the other midwives had endured, let alone the community of mothers here in this corner of Africa because their arms were empty.
I don’t know how to describe just how far St. Theresa Mission Hospital in Nzara has come over the past five years since the start of the construction of the Maternity Unit and Operating Theater. The level of loss was far more significant than it is now. Mothers wouldn’t be able to get to the clinic because the roads were unsafe during the war, or washed out from rain storms. If there was an emergency, we frequently had to send the laboring mother an hour’s drive away to the nearest hospital over rough terrain – and that was only when it was light out and the roads were safe enough. A baby’s life expectancy frequently depended on the weather—if it was a sunny, warm day, the baby might stay warm enough to survive. We would have solar power so the baby could receive oxygen if needed. Babies born on cool, cloudy days were less likely to make it, and back then we had no incubators to keep them warm. The solar panel batteries would run out in 2-3 hours, so if a baby needed oxygen, they could only have it for a short time before the power ran out.
I remember vividly feeling this hopelessness on a cold and overcast day as I heard the beeping sound alerting me that the batteries were about to run out. I then had to disconnect a small newborn boy from his life-saving oxygen and place him into his mother’s arms. The power had run out right when he needed it the most. His precious life lasted a little under 3 hours after that.
After constructing the Maternity Unit and Operating Theater in Nzara, we placed healthy babies into their mothers’ arms more frequently than before. St. Theresa Hospital was now able to provide emergency c-sections around the clock for any obstetric emergency, responding quickly to complications that previously would have resulted in a loss. After a solar power expansion in April 2023, the number of newborns that left the hospital healthy increased further. We could now provide oxygen around the clock to babies who needed it. The incubators could now run nonstop. Reliable incubators, combined with Kangaroo Mother Care (skin-to-skin contact between mom and baby), meant we could keep babies almost as small as two pounds alive.
For me, it was a humbling experience getting to watch this revolutionary change unfold in Nzara. Now that we were able to provide oxygen with our resuscitation attempts, babies, whom, five years ago, would not survive more than a few hours after birth were now able to leave the hospital healthy—their mothers trained on the importance of skin-to-skin care and breastfeeding.
Right after we got reliable power at the hospital, we had a mother deliver her baby in our facility. She was having a difficult labor at a smaller facility called a PHCC (primary health care center) and was referred to us. She delivered her baby shortly after arriving, but her baby wasn’t breathing.
The midwife and I quickly brought the baby to the resuscitation table. We were able to immediately deliver oxygen to the baby while trying to revive her with a bag and mask. I heard the baby’s family start fervently praying as we resuscitated their little one. The baby’s body slowly changed from blue to pink, but she still couldn’t breathe alone. Suddenly, the baby girl took a massive breath and let out a loud cry that pierced through the mask she was wearing. Her aunt and grandmother collapsed in complete shock and awe at that sound, and the mother and family all started crying in thanksgiving for her survival. Up until now, families in this situation expected the baby to pass away, used to the fact that there were minimal resources. Now, I have the honor to see, time and time again, mothers and families expressing their shock and joy that their baby survived a situation that would previously hold death.
I get to watch mothers peer at their tiny premature babies in the incubator in amazement that their three-pound baby survives one week; then two weeks, three weeks, and eventually, is healthy enough to go home. The mothers are eager to learn how to care for their tiny babies through classes about skin-to-skin care, cup-feeding their babies with expressed breastmilk, and caring for their premature babies at home. They have hope that their little one can now survive.
The Nzara community around the hospital is thriving as well. Now that people are traveling from all over Western Equatoria for the care we can provide, the village’s homegrown goods are being bought and used by all who come to bring their loved ones to the hospital. Where once people of Nzara primarily lived in houses made of handmade brick and grass roofs, they now can afford to build their houses out of concrete and even have metal roofs.
There is joy at every breath. Life is replacing loss, and mothers are joyfully carrying their babies home alive. The work is always ongoing, but tiny changes, hard work, and sacrifices have led to this incredible leap of life that fills Nzara today.
CMMB has supported the delivery of care at St. Theresa Hospital since 2012. Thank you to our coalition of partners that make this support possible: African Mission Health Foundation, Aurora Humanitarian Initiative Foundation, Friends of St. Theresa Nzara, and Sudan Relief Fund.
Together, we’re expanding access to healthcare for the people of South Sudan.