What is Long COVID? A Doctor and Patients Explain
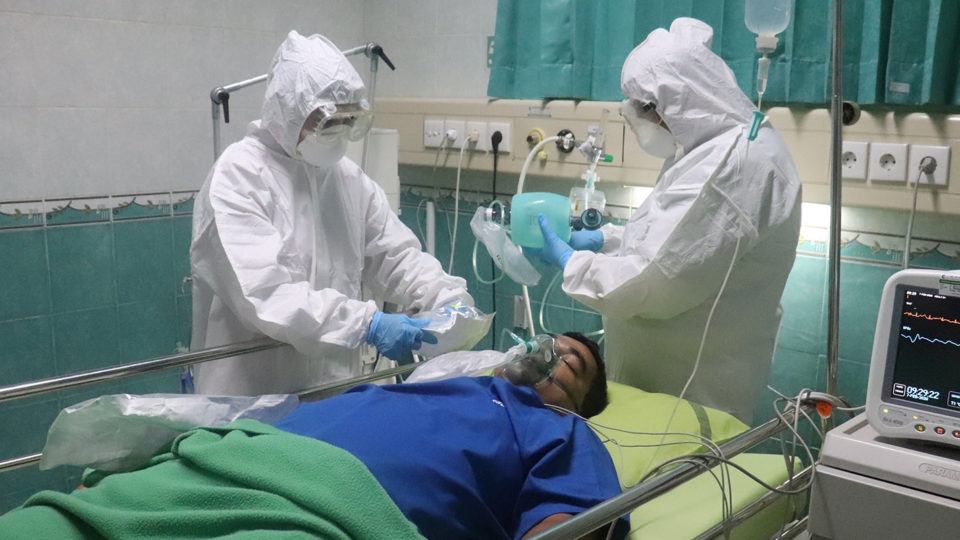
After eighteen months, COVID-19 continues to wreak havoc across the world, and we continue to learn more about the evolution of this disease. Many people who have recovered from COVID-19 still experience some symptoms months after the infection; often known as “long COVID.”
Dr. Helene Calvet, CMMB volunteer and infectious disease specialist with over 20 years of experience in local public health including COVID-19 response in Orange County, California, joined a panel discussion to describe what is currently known about the short and long-term effects of COVID-19. Guest speakers also included patients who shared their powerful experiences living with long COVID. The discussion was led by Dr. Claudia Llanten, CMMB’s senior specialist in maternal and child health with over 19 years of experience in global health.
Dr. Helene Calvet Explains Long COVID
Can you tell us about your work during the pandemic?
For the last 18 months, I have been in charge of a team of nurses that have responded to COVID outbreaks in skilled nursing facilities and older adult residential facilities in Orange County, California. We responded to over 300 outbreaks that infected thousands of residents and staff. We have a lot of experience diagnosing COVID and recognizing COVID. We have seen plenty of long COVID in the nursing homes.
What is long COVID?
Before I talk about long COVID, I want to give some important caveats. Number one is that you really can’t describe well something that is not defined. Unfortunately, long COVID is not defined. Experts have not agreed upon a name or case definition for the syndrome of persistent COVID-19 symptoms.
There are no standard case criteria—like how many symptoms you must have, what types of symptoms, what time period. It seems that most studies agree that symptoms after about four weeks indicate long COVID. Some would break that down into a sub-acute phase which lasts from four-to-twelve weeks and a more chronic phase which goes beyond 12 weeks.
The bottom line is that symptoms continue or start after the acute illness is over, so the symptoms may just be ongoing, or they can come and go. Interestingly, new symptoms that someone didn’t experience during acute COVID may appear weeks to months after that acute illness is over.

Dr. Helene Calvet is a CMMB volunteer and infectious disease specialist with over 20 years of experience in local public health.
What are the symptoms of long COVID?
The most common general symptom seems to be fatigue. This seems to be a tiredness that is worse than what is normal. Other common symptoms that seem to come out through many studies are headache, shortness of breath, and then mental issues—difficulties concentrating and with memory.
There’s a whole variety of symptoms that have been reported. They can involve the lungs, heart and blood vessels, hormones and the glands that produce them, brain and nerves, kidneys, skin, stomach and intestines, and muscles and bones.

A diagram of the long-term effects of COVID-19. (Source: Scientific Report, 2021; 11:16144)
Are there treatments for long COVID?
There is no specific treatment for this. There is no medication. There are some approaches to a sort of gradual reintroduction of activity and certain things that can help. Since it is so ill-defined, there is no definitive treatment for this.
How do vaccines relate to long COVID?
Worldwide there’s been over 4.5 billion doses given. They are safe!
Yes, everything in life has potential side effects or potential risks, but in this case, the benefits far outweigh any risks. They’re very effective at COVID. Although breakthrough infections are occurring due to the Delta variant, fully vaccinated people are much less likely to have severe disease, end up in the hospital, or die from it than are unvaccinated people who get Delta.
If you don’t get COVID, you can’t get long COVID. If you have not been vaccinated or if you have friends who have not been vaccinated yet, I highly encourage them to get vaccinated as soon as possible.
As of September 2021, billions of vaccine doses have been administered worldwide, equal to 75 doses for every 100 people.
How common is long COVID?
Estimates vary widely, but it seems it’s common among hospitalized patients and less common among those who are not hospitalized. We don’t really have a good estimate how common it is among people who didn’t have any symptoms at all initially. It is definitely more common among those who are sicker or had more symptoms. One study that I read said that if you have five or more symptoms of COVID initially, then you are more likely to have long COVID.
It also seems to be common with those who are older, those who have more medical conditions, and more common in women than in men.
Are people who experience long COVID still contagious?
No. This ongoing syndrome of symptoms does not indicate that someone is contagious. We know that the test can continue to be positive for three months. That’s because the PCR tests are so sensitive. They pick up just little bits of broken-down virus that the body can be clearing out for several months after infection. It doesn’t mean if someone has a persistent cough or persistent fatigue that they are still contagious.
Patients Share Personal Experiences Living with Long COVID
Patients living with long COVID joined the panel to give testimonies on their experiences. The guest speakers included Constanza Tobasía-Hege, a microbiologist, medical doctor, and public health specialist with more than 15 years of experience, a CMMB health facility staff member, and CMMB community health worker.
Can you tell us about your experiences living with long COVID?
Constanza:
I got infected with COVID in December 2020. Even though I had very mild symptoms—a little headache, very low fever —after a week feeling better, I started developing weakness and tingling in my hands and in my arms. It quickly surpassed that level to reach paralysis, lack of control of the movement in my four extremities. I lost the ability to walk. I lost the ability to move. I lost total control over my body. I was still feeling pain and discomfort which was something very difficult to manage. I was totally aware of what was happening to me, but I couldn’t even speak. I lost the ability to swallow, to chew. I also developed Guillain Barre syndrome, which is an immune disease that affected peripheral nerves in my entire body.
I was hospitalized for a month. Two weeks of that time, I spent in the ICU everyday facing death with the fear of long-term disabilities. It’s been nine months, and my right arm is still paralyzed. I’m right-handed so you can imagine how difficult life has been for me during this time.
There are really no words to express the dimensions and the different aspects of life that are the long-term consequences of COVID for a person, for a family, for employees, for the health system, for an entire country’s economy.
There is a lack of capacity, especially in undeveloped countries, to respond.
In my personal life, after a month of being hospitalized facing difficulties, I came back home in a wheelchair and started little by little the process of learning again how to swallow, how to speak, how to move my face, how to walk, and how to use my arms again. I haven’t been able to go back to work because I’m still dealing with everyday therapy. I have physical and occupational therapy. I have regular checkups and tons of medicines to take every day. To be sincere, my whole life has been turned upside down.
Depression, anxiety, and mental health difficulties bear on my life and my family. I’m a wife and I’m also a mother. Even as a doctor, I never expected this disease to be so cruel, so long-lasting, and so devastating.
Besides the personal barriers I experience, there is a lack of ability in the health system to deal with this terrible pandemic. There is a lack of capacity, especially in undeveloped countries, to respond to all the other barriers that a person in my specific case—a person with disabilities and being handicap—faces.
Health Facility Staff:
After being hospitalized on oxygen for nearly a week, I was discharged and went back home. For the next two weeks, I struggled with severe malaise and cough. My COVID tests remained positive after three cycles of testing every two weeks. The biggest struggle for me was insomnia and being startled, which I dealt with for the next three months. I regained complete function after three months.
My strong support systems—especially my family and friends—played a big role in managing the stigma related to COVID.
The insomnia and hallucinations were the most difficult to deal with, especially since my role requires me to be mentally alert and to be able to provide thought leadership. First, my colleagues were very supportive and allowed me to work from home, especially during the time that I was still recovering from the physical symptoms. I opted to resume work because being away from work also affected me. Engaging in work-related tasks helped me regain some normalcy, especially when struggling with the hallucinations. Second, my strong support systems—especially my family and friends—played a big role in managing the stigma related to COVID.
Community Health Worker:
I work as a community health worker and I’m also a mother. I used to walk a lot, quick and without any problem, for kilometers. When I started to recover, I realized that I could not walk for more than a few meters before getting tired. I had to rest for a while to be able to continue walking. I thought, “Could it be because I’m using a new mask? Or could it be that COVID left me this way?” I felt mostly recovered by March, but a month later I started coughing again, almost daily. Since then, my cough has continued, and I still get tired easily. Now, my tasks take more time, but I need to be patient with myself.
Do you have a final message about long COVID?
Constanza:
I would like to emphasize the role of prevention. I think there is this big work being done by health systems which is very important, but the role that we have has individuals—as family members, as coworkers, as a regular person in everyday life—is also important. We can promote a culture that is against stigmatization, a culture of talking openly about COVID. We can promote the need to wear masks properly all the time in every place. We can promote vaccination for people who have vaccines available.
For us dealing with the long and very devastating consequences of COVID, it is unacceptable for people to refuse to get vaccinated or to promote conspiratorial theories that undermine public health practitioners around the world. I think it’s very important to do as much as we can as public practitioners and community health workers, but also as regular people to encourage a culture that accepts COVID as a threat to humanity and deals with it in the ways that we can: hand-washing, physical distancing, the proper use of face masks, and especially vaccination.
This would be my message. I don’t want anyone to have to walk the path that I have walked these past nine months.

The use of face masks, hand-washing, and physical distancing are all important practices to prevent the spread of COVID-19.
Health Facility Staff:
What we have learned during the time of COVID should help us re-think what kind of support we can provide to specific teams. The “one size fits all” approach may not be entirely sensitive to the needs of all teams in an organization. Perhaps this may require focus group discussions with different teams to understand the emerging needs and how they can be addressed.
My last point is prevention. If you want to help your family, communities, friends, and colleagues—take care of yourself by following preventive measures, including stress management.
Community Health Worker:
When I saw in the news how many people were dying from COVID-19, and then people close to me and people I knew also died. That made me think, “We can be fine today, but who knows what will happen tomorrow?” Before having COVID, I thought, “Why follow all these guidelines, if I did not have it and nobody around me had it?”
But this year, after having COVID, I understand that it is something really ugly. I completely lost my appetite. I couldn’t smell. People were afraid to be close to me. All this has made me reflect, it may be at random that God selects us, but I feel that God gave me an opportunity. Many people have died. I am thankful that I did not go to another life. We must value life, and continue taking care of ourselves, following the preventive measures that we can. It’s not just me, we must all take care of our family and others. As community health workers, we need to talk with young people. They go out on the street, so they can be asymptomatic and bring this disease home. But at home, we have other loved ones—dad, mom, grandparents, children. I was the source of infection in my house, and my mother was infected through me.
To stop this, we really need to work worldwide to get everybody vaccinated.
Dr. Helene Calvet:
I really wish that everyone could hear this and believe that this is a serious issue—and get the vaccine and help to promote the vaccine because that’s ultimately the answer. [The pandemic will continue] until the whole world—I mean, everybody—has access to this vaccine. If we don’t, if other countries that are lower resource have less access to the vaccine, the new variants will come up. Until every country has high levels of vaccination, new variants will come up and there’s nothing to keep those new variants from spreading around the world. To stop this, we really need to work worldwide to get everybody vaccinated.