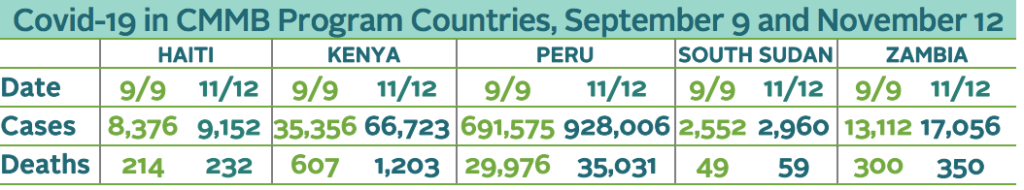
COVID-19 Situation Report – November 2020

Deep Into the Pandemic, Its Final Toll Is Still Unknown
Since the early days of the pandemic, CMMB has been coordinating with our country offices to provide lifesaving medical supplies and PPE to under resourced health facilities, all while redesigning our approach to ensure our ongoing programs can continue amid the pandemic. In our latest situation report, we detail the virus’ impact in each of the countries we serve as of November.
Working Towards the Health of the Most Vulnerable
Even as a rise in COVID-19 incidence appears to have stalled in most of the countries we serve, the death in Lima, Peru, of a five-year-old girl of diphtheria—a disease preventable by a well accepted and effective vaccine—tragically highlights a corollary risk of COVID-19: The stigma around it and broad fear of sickness keep families from seeking lifesaving services at health facilities.
Community health workers have put in long hours over the years helping families understand why child immunization, antenatal care, and other resources available at health facilities matter. The current challenge is to continue delivering this important messaging while conveying the COVID-19 information that families need. Community health workers are meeting this challenge despite fears for their own safety—and the safety of their families. We are daily grateful for this work.
Haiti: Cautious Optimism
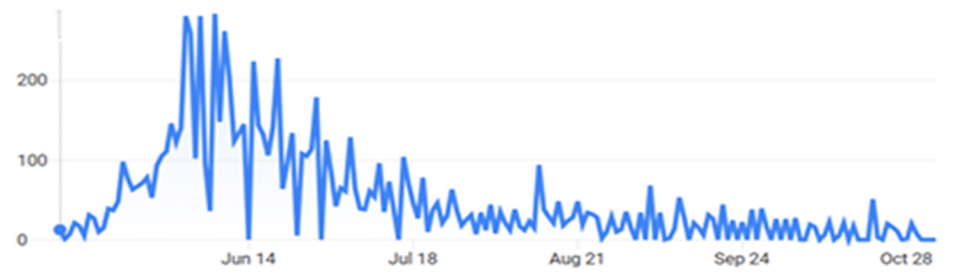
The pandemic has not brought on the disaster that many feared for Haiti. Perhaps it is because so few foreigners travel there, by comparison to its easterly neighbor on the island of Hispaniola, the Dominican Republic, the Caribbean’s COVID-19 epicenter. Perhaps it is because of the youth of Haiti’s population; 54 percent of Haitians are younger than 25, and the median age is 23, compared to 30 globally. Then, too, Haitians live an open-air lifestyle. Homes are small and families large. People spend their time outside, and when they’re inside, the windows are open.
Stigma and misinformation: Misinformation about the virus has created stigma around it—“greater even than for HIV,” observes country director Dr. Jean-François, who also runs one of Haiti’s most successful HIV programs, with U.S. Centers for Disease Control and Prevention funding. Some Haitians believe that COVID-19 is spread by community health workers, known as agents de santé communautaire polyvalents (ASCPs; polyvalent health agents). Some parents refuse to bring their children for immunization. Patients fear retribution from neighbors. In remote, impoverished Côtes-de-Fer, healthcare staff briefly moved from homes in town to the hospital guest house because of hostility against their contact tracing.

At the Bishop Joseph M. Sullivan Center for Health in Côtes-de-Fer, all visitors wash hands on arrival and wear masks. Opened in 2017, CMMB’s hospital was built thanks to the generous support of donors.
Multifaceted response: CMMB actively collaborates with faith leaders—priests, pastors, voodoo practitioners—to give them correct knowledge of COVID-19 as well as the skills to communicate the facts to their followers. In addition, we support Haiti’s national lab in its surveillance activities, including training of surveillance officers to monitor community transmission.
“COVID is playing yo-yo in Haiti. One day you have 30 cases, another three. Many people are out and about without masks, not staying vigilant or taking precautions.” —Dianne Jean-François, MD, MPH, Country Director, CMMB Haiti
We have also been active in Côtes-de-Fer. Beyond creating new COVID guidelines for ASCPs and training them, we worked to sensitize community members on COVID-19, met with local leaders to chart a coordinated response, and broadcast COVID-19 messages on local radio. As needed we replenished the personal protective equipment (PPE) already distributed to ASCPs, motorcycle drivers who provide local transportation for the community, and the agricultural agents that CMMB brought on board to work with local families to cultivate crops and raise goats. The potential for a second, more vicious wave of infections is never far from the minds of CMMB staff members as they travel, masked, to their work places every day. There is a sense of waiting for the other shoe to drop, all while they hope that it does not.
Kenya: Hard-Won Gains Wiped Out
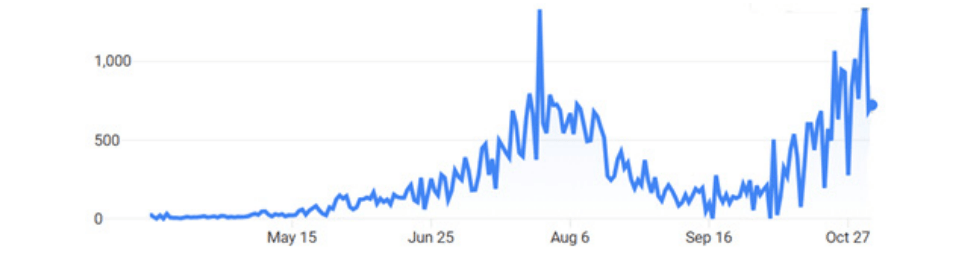
Kenya has experienced far fewer coronavirus deaths than other nations with similar infection rates—only 1,203 in a nation of 50 million since the virus arrived in March. Epidemiologists pin the nation’s youth as one cause—half of Kenyans are younger than 20 and only 4 percent are 60 or older. Youth cluster in cities; elders retire to rural areas. Life is lived outdoors; indoor spaces are ventilated well. Incidence is low of noncommunicable diseases that create risk for severe COVID-19 infection.
That said, after bottoming out six weeks ago, COVID-19 is on an upswing. Fearing getting infected during delivery in an urban health facility, pregnant women are traveling to the countryside to have their babies. In response to the surge, government is doing mass testing and mandated the counties to enforce masking up, social distancing, hand-washing, and bans on gatherings of more than 15 people. Observing that months of gains had been wiped out in eight weeks, President Uhuru Kenyatta announced continuation of Kenya’s nighttime curfew until January and local lockdowns where needed.
“Counties did a lot during the first wave to raise preparedness, investing in PPE and training for health workers. But with the surge in COVID cases, with the county level rise in mortality, a second wave in Kenya would be dire.” —Jesse Kihuha, Project Manager, CMMB Kenya
Dangerous soup: All this is against a backdrop of grinding coronavirus fatigue and a crippled job market, a situation so dire that the United Nations’ World Food Programme has rolled out cash transfers and nutrition relief to 400,000 people in hard-hit Nairobi and Mombasa. With schools open just for classes with moving-up exams, teens are at risk for early sex, drug, and alcohol use. “We may have lost a generation,” says CMMB country director James Kisia, MD. He and project manager Jesse Kihuha view the status quo as a “dangerous soup,” describing deadened sensitivity around messaging; mistrust of health institutions and government; weak infrastructure to track, refer, and manage cases; and the potential for disastrous transmission to elders after urban job losses drive asymptomatic, superspreading youth away from cities. Add to that politicians anticipating 2022 elections, who are out shaking hands, unmasked and undoing sound government messaging.
Ahead of the curve: Step by step, CMMB is continuing to strengthen the health system in our CHAMPS catchment, vulnerable Kitui South Sub County, toward a strengthened COVID-19 case management capacity. A sand dam near Kanziko has just been dug; as soon as electrical mechanical work is completed, it will collect rainwater runoff for subsequent purification, storage, and piping to Kanziko and its health center. Like Kamutei health center maternity ward (pictured in our last sit rep), Kanziko’s will soon have fresh, clean piped water.

CMMB Kenya provided Kitui South’s main treatment center with changing rooms for changing in and out of PPE.

Deaths are surging among healthcare workers. To protect them, we have installed a sanitation booth at the Kitui South treatment center. The booth removes virus and bacteria on clothing and minimizes transmission of infection.
No gaps in immunization: Reverse migration from cities has flooded rural areas with nonimmunized children; CMMB immunization drives have surpassed targets and reached more children than ever. We supported health facilities with gas to maintain cold chain. When one fridge nearly ran out, CMMB stepped in.
Workforce protection: Most facilities have just one staff, a nurse. To minimize these workers’ exposure to COVID-19, we deployed community health volunteers to go door to door giving vitamin A and deworming to kids under five. Thus, only the underimmunized will seek routine services at facilities.
Peru: Respite before the second wave
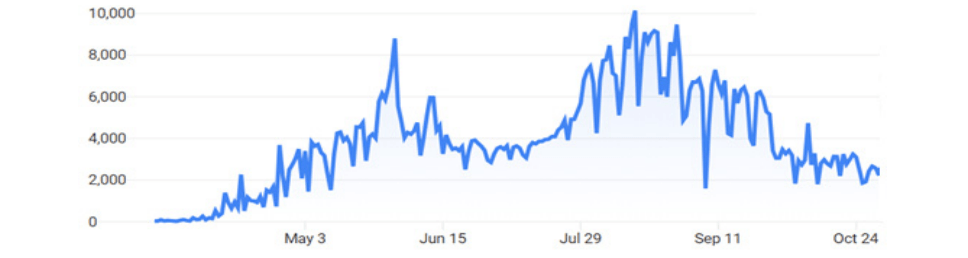
Peru’s epidemic has been one of the Americas’ worst; its mortality is the world’s highest after tiny San Marino. Consequently, Peruvians heaved a sigh of relief to hear in mid-October that the weekly coronavirus infection rate had dropped fully 50 to 70 percent in some regions, up to 36 percent in the capital. The great 15th-century Incan citadel, Machu Picchu, reopened, a boon for Peruvians whose livelihoods depend on tourism. Yet growing talk of a second wave has been worrisome.
“Most Peruvians have a mental health challenge to address. We have friends who have died, and so we live with a kind of paranoia or depression. A high number of healthcare professionals have died. They are young, productive, with a long future ahead of them. We know that the people we work with feel not so good as well. We are going to have to become accustomed to living with this for a while. And families are afraid, and living with sorrow.” — Ariel Frisancho, MD Country Director, CMMB Peru
As prevention, President Martín Vizcarra extended the restrictions aimed at viral containment—the ban on larger gatherings, the nighttime curfew, and the mandatory wearing of face masks in public. Also announced was provision of a second Universal Family Bonus, $223, to 4.2 million households. The health system is ready—to a point.
“We have a modern, mostly equipped health system in Lima city. The same can be said of Trujillo and Huancayo cities. But inequalities are stark, and access for the poorest is limited—it’s a question of who gets to the hospital, who gets into the emergency room, who gets a bed.”—Ariel Frisancho, MD Country Director, CMMB Peru
Routine healthcare: Immunization coverage, close to 90 percent in CMMB’s CHAMPS catchments and across Peru in 2019, plummeted with the pandemic—to 40 percent nationally. Public health advocates see the death of the Lima five year-old, the first from diphtheria in 20 years, as a concerning harbinger; three relatives were subsequently diagnosed, plus one other. The girl had received her initial shot, but no booster. The ministry of health responded with vigorous immunization campaigns. In the areas where we work, CMMB phone chains have helped get the word out while following up on children with anemia and pregnant women. In addition, community health agents have made specific efforts to visit families who have fallen out of touch or where child health issues were a possibility. COVID-19 has expanded our outreach toolkit to phone calls, video chats, and WhatsApp groups, enabling us to reach 15,109 people since February.
South Sudan: Setting up for Success
In South Sudan, the worst flooding in six decades has submerged villages and fields, killed livestock, and displaced whole communities to Juba, COVID-19’s stronghold in South Sudan—all while insecurity in high-burden neighboring countries is sending additional waves of refugees into South Sudan. Testing is now decentralized to Yambio, Nzara, and other locations, but it remains low overall. Although 24 of the nation’s 80 counties now have cases, the numbers are low overall. Few individuals have lost loved ones and do not see COVID-19 as serious and life threatening. So many South Sudanese ignore measures set by the government. Churches and schools are open.
Fear of a strengthening epidemic: Given the situation, there is fear in public health circles that even the smallest change—for example, a viral mutation— could exact an immense toll. Long civil war has weakened South Sudan’s health system, and most facilities are unequipped to manage an onslaught of patients requiring intensive clinical care.
CMMB—An active partner: CMMB is focused on supporting national and county efforts to bolster preparedness, and we are active on task forces, technical working groups, and a steering committee aligning partners’ activities. Response mechanisms created during an Ebola epidemic have been revived.
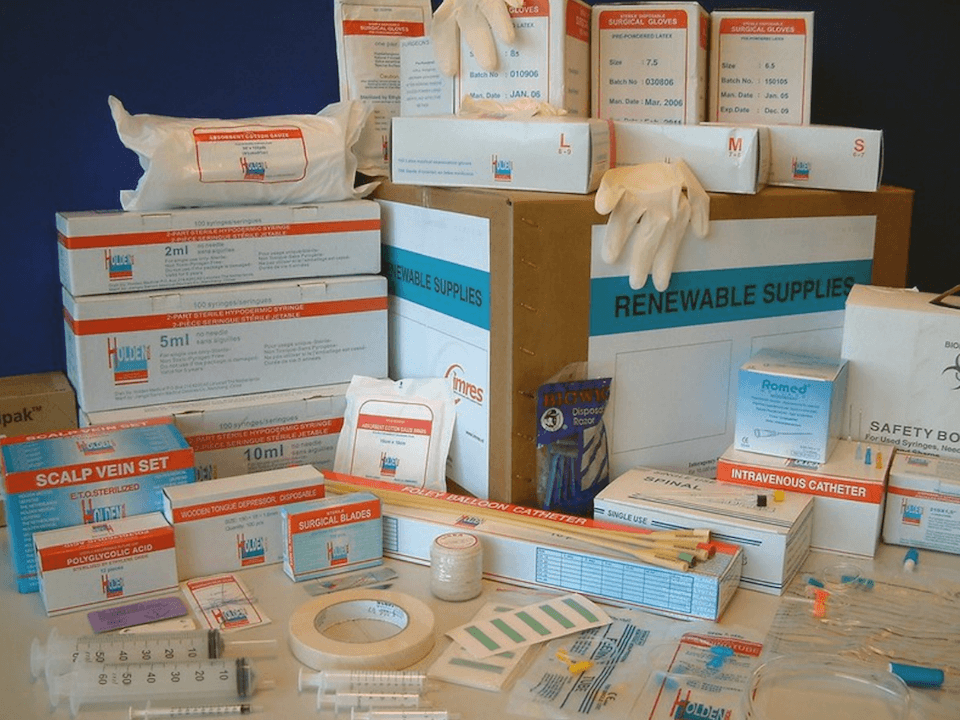
CMMB’s Medical Donations Programs regularly ships high-quality medical supplies to partners in the western Equatoria region.
Water works: Having installed the region’s first permanent handwashing blocks at three hospitals in spring, we repaired the water line and provided solar power for the hospital pump in August; these benefit the local community in addition to the hospital. In September, we installed a 5,000-liter tank at Yambio State Hospital; the tank provides water for 5,000 people weekly and 200 hospital staff daily.
Now, in addition, we are resuscitating an isolation center in Ezo, near the border with Central African Republic and Congo; developing another in Nzara; and managing a third, a 16-room former guesthouse renovated by the United Nations Mission, in Yambio, with support from the United Nations High Commission on Refugees, which dug a borehole at the site. We are training workers, establishing linkages with other players, and acquiring resources needed for operationalization. At the same time, we are providing supplies of hand sanitizer, face masks, and other PPE to health facilities in Nzara, Ezo, Yambio, and Lirangu, and maintaining the handwashing blocks and triage centers. These have proven effective at capturing cases while serving as a platform for educating hospital visitors on COVID-19.
“Preparedness is lagging somewhat. Areas are vast, and transport and communications are an issue. Having critical care only in Yambio is not sufficient for our population.” — Edward Bepo, MBBS, MSc, Emergency Preparedness Technical Adviser, CMMB South Sudan
Zambia: Wait and See
Despite spikes, life in Zambia returned to normal over the summer. People felt COVID-19 was going to be managed and got used to living with it. Zambians went back to offices and schools opened. Bars poured, although on a weekends-only pilot basis. Churches filled, even as government messaging advised masking up and social distancing. In markets and on transport, it’s been business as usual. World Health Organization data noted that three quarters of Zambia’s cases are asymptomatic, with patients sent home to be cared for by their families under guidance from community health workers.
“Masks are for sale on every corner. Everywhere you turn people are selling them. Most are washable and reusable, so people do not need so many. Also, people are relaxing, not seeing the need to buy masks. In May, stores would not allow you in without a mask. Now, not so. We are continuing to watch the space and hope that it doesn’t get bad.” — Chanda Kaibele, Finance & Grants Officer, CMMB Zambia
With high national HIV and TB rates, Zambians are accustomed to living with an epidemic, so many are knowledgeable about infection prevention and control. Such home-based case management has minimized stress on health facilities and isolation centers. Around Mwandi, the focus in Zambia of CMMB’s signature CHAMPS program, only a handful of cases have been seen; nearby Sesheke has had some.
Strengthening communities: CMMB continues to support communities’ prevention efforts by ensuring that families have water for handwashing. Of eight planned wells in the Mwandi area, we have completed four, and the others are scheduled for completion and handover at month’s end. Trainings for community health workers have been ongoing, incorporating information about the novel coronavirus.
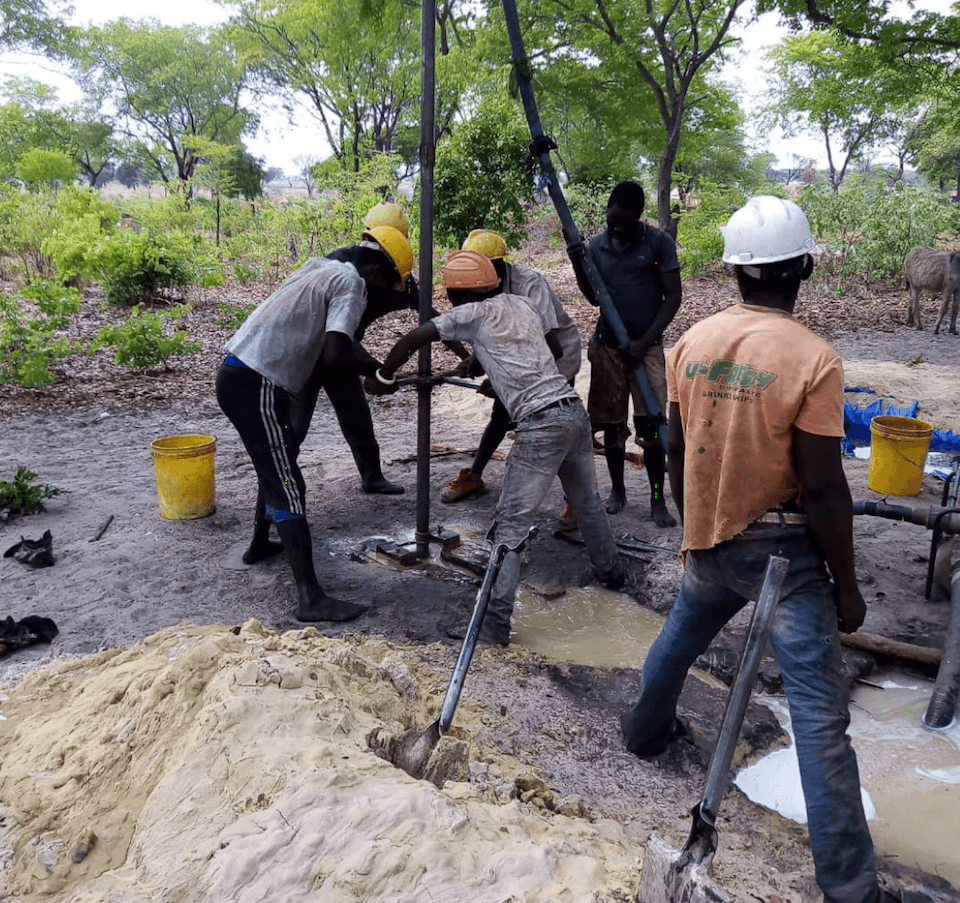
Hand-digging a well takes teamwork. By late November, access to water will be easier in eight localities near Mwandi, thanks to CMMB donors.
Ongoing good works: In the north, where a CMMB project seeks to mitigate gender-based violence, activities in the community and among health workers have continued. In Lusaka, parents of adolescent girls and young women involved in our DREAMS project—parents once leery of letting daughters leave their homes—have eased up. However, the mask-making project initiated early in the epidemic by a group of these enterprising girls has scaled down in the wake of low demand and high supply.
Thank You To Our Donors
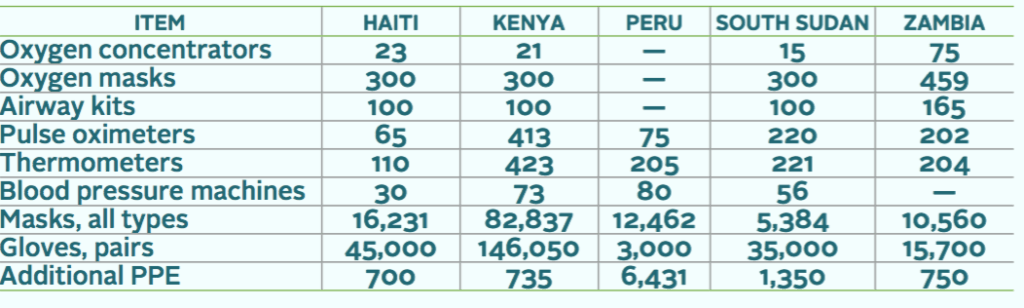
Donors make our ongoing programs and emergency intervention possible—including our expansion of critical water access for health facilities and their communities. Their ongoing support has also enabled us to help prepare our country offices with the medical supplies and equipment that will be needed in supported catchments to meet the challenge of the pandemic. Since the early days of the pandemic, we have shipped or facilitated the local or international purchase of thousands of essential items.
Most recently, after a CMMB assessment revealed community health workers and health facilities were ill prepared for outbreaks, we dispatched three-month quantities essential to COVID-19 case management. Our Medical Donations Program maneuvered within a context of great shortages and stressed global supply chain to meet the great need, and we will continue to do so as long as required.