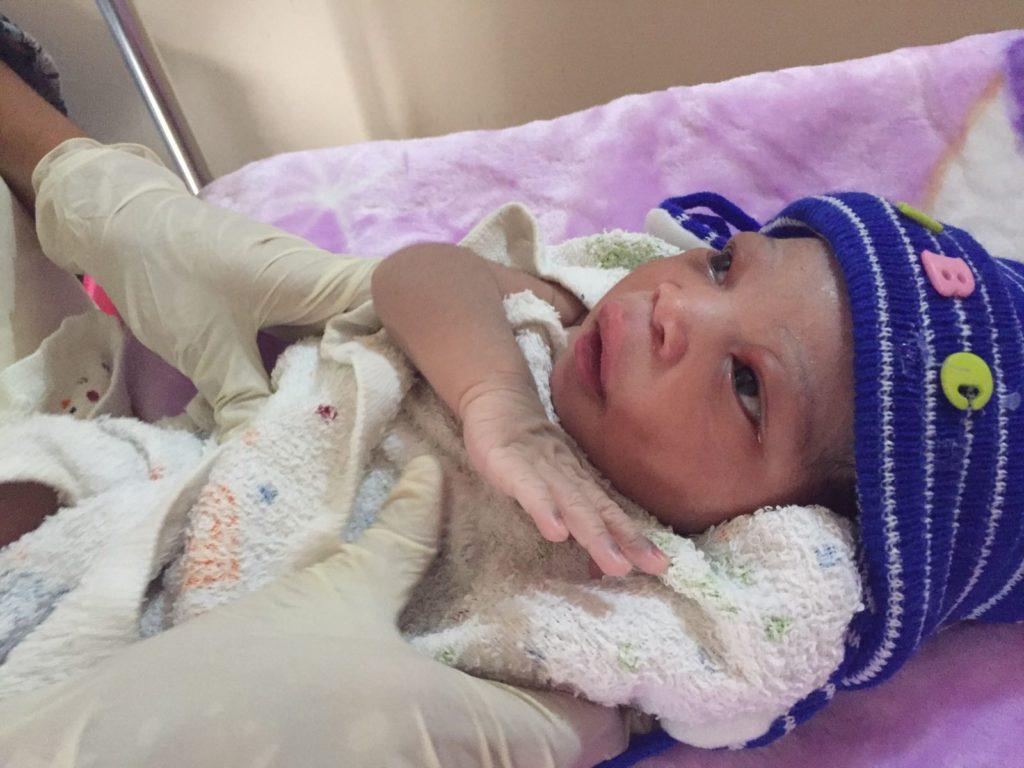
Counting to Moja: An International Volunteer Deals with Loss

Dr. Mary Fleming is a self-professed nomadic doctor. She is a US-trained OB/GYN who travels around to provide care in different parts of the country. But her most recent placement has taken her much further afield. She is currently serving as a volunteer with CMMB in Mutomo, Kenya. In this blog post, Dr. Mary talks about the reality of infant mortality in this remote and impoverished area of Kenya.
Remembering the Ones We Lost
Typically, my clinical responsibility ends at birth.
When all things go well, after guiding the mother through prenatal care, labor and delivery, I happily hand off the new bundle to the awaiting nursing or pediatric staff. I congratulate the parents and wish the baby a “happy birthday”, before exiting the room to complete my notes.
Here in Mutomo, my responsibility is not always over at birth.
Normal newborns with no issues are assessed at birth and then discharged with their mothers to follow up as outpatients. However, we admit those neonates with complications and they become part of the maternity service, (i.e. my service).
As you can imagine, I had to tune up on my newborn medical knowledge.
No Heartbeat, No Respiration, No Longer…
My second week on service, as I finished rounds, I was called to evaluate an infant who had been doing poorly for the last few days. He had been diagnosed with meconium aspiration and neonatal sepsis. The treatment regimen included antibiotics and supplemental oxygen.
Over the previous few days, he had increasing difficulty breathing and maintaining his oxygen levels. One of the nurses was actively trying to resuscitate the infant when I arrived; I assisted but felt at a loss in offering any additional support. As we watched the oxygen saturation levels drop into the 30’s, the infant was barely responsive to stimuli and losing muscle tone. I asked for one of the other doctors to come to assess the situation, he then relieved me so that I could report to the operating room for a case.
I learned soon after that the infant was pronounced dead. A few weeks later, I was walking past the maternity unit on my way to dinner and I heard, “Dr. Mary, can you stop in?” One of our admitted infants, born to a mother the day before after a difficult vacuum assisted delivery, no longer had a heartbeat, no longer showed any evidence of respiratory effort, no longer…
She called me to write the note to certify death.
As an Ob/GYN here, we handle difficult situations more often than we would like. I have diagnosed miscarriages and stillbirths however this was the first time I pronounced death after delivery. The discussion of a death of child with a mother, whether at 8 weeks, 36 weeks or two days after birth is difficult.
It doesn’t get easier with time. There are no consoling words.
Infant Mortality: The Difficult Facts
During residency and then as a public health student, I developed an interest in how I could work to reduce infant mortality, both locally and globally. One of the health predictors of a country is linked to how well the newest members of its population fare after birth.
More specifically, infant mortality is the number of infant deaths before a child reaches his/her first birthday.
Globally, the infant mortality rate has decreased from an estimated rate of 64.8 deaths per 1000 live births in 1990 to 30.5 deaths per 1000 live births in 2016. Annual infant deaths have declined from 8.8 million in 1990 to 4.2 million in 2016. – WHO
As advanced as healthcare is in the United States, we still do a sub-par job in protecting one of our most vulnerable populations. In 2010, the infant mortality rate in the United States was 6.1 deaths per 1,000 live births. Compare this rate to Finland 2.3, France 3.6 and England 4.1.
In Kenya, the infant mortality rate is 38.3 per 1,000
The discrepancy between populations in the United States is even more disheartening. We see a large gap in the rates of infant mortality between white and black women; the most recent data reveals a rate of 11.3 (which translates to a ratio of 2 to 1).
One way to combat this problem for me clinically is to provide comprehensive, appropriate care for women, especially women of reproductive age. The best prenatal care starts at pre-conception and continues into the pregnancy.
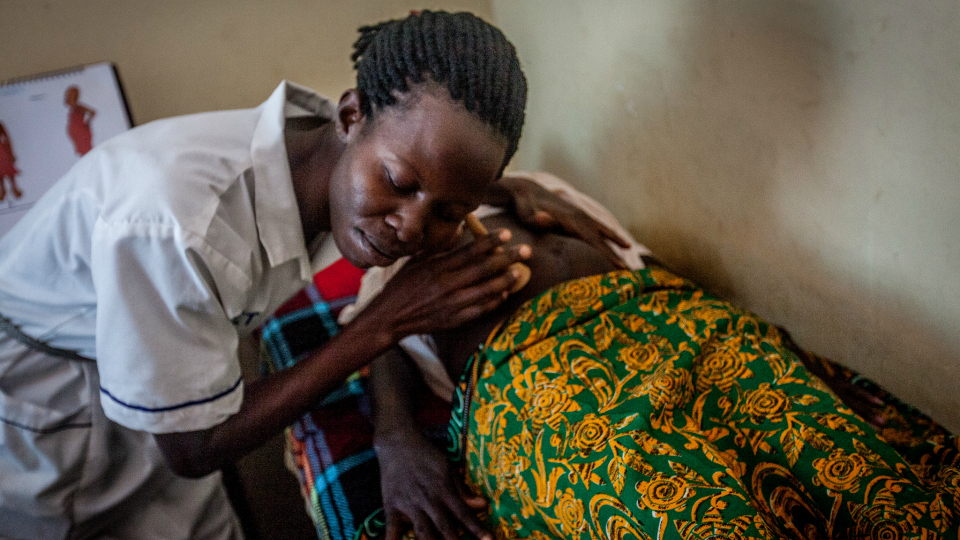
The most important medical check-ups of a baby’s life happen before she’s born. Ensuring pregnant women receive prenatal care is a priority.
However, we know that adequate medical care is not sufficient and even when controlling for education and income, black women in the US still have increased rates of infant mortality. Studies have confirmed that stress plays a factor in these outcomes, especially the stress due to the consequences of racism in the United States. (See the link to the PBS special entitled Unnatural Causes).
In Kenya, the infant mortality rate is 38.3 per 1,000. According to the WHO, “the main causes of newborn deaths are prematurity and low-birth-weight, infections, asphyxia (lack of oxygen at birth) and birth trauma.”These causes account for nearly 80% of deaths in this age group.”
CHAMPS in Mutomo
CMMB through its CHAMPS (Children and Mothers Partnerships) program has collaborated with Mutomo Mission Hospital to combat this situation in sub-county of Kutui South. Interventions include:
- promoting antenatal care,
- training community health volunteers,
- supporting community health centers,
- providing equipment and supplies,
- in addition to enlisting the aid of volunteer doctors and nurses.
I can see the results of this program when taking the history of our patients in labor and delivery. Women who have traditionally delivered at home are now seeking care in a skilled facility and pursue referral earlier if complications arise.
The public health community has made great strides to reduce infant mortality and the rates have decreased. But there is still much work to be done at home and abroad.
Though I don’t have any biological children, I experienced pregnancy and childbirth alongside two of my closest friends. I am now blessed with two godchildren who are healthy and happy.
I hope my work, in some way, allows more women to experience the same blessings.